Quantification of head and neck cancer patients’ anatomical changes during radiotherapy: Toward the prediction of replanning need
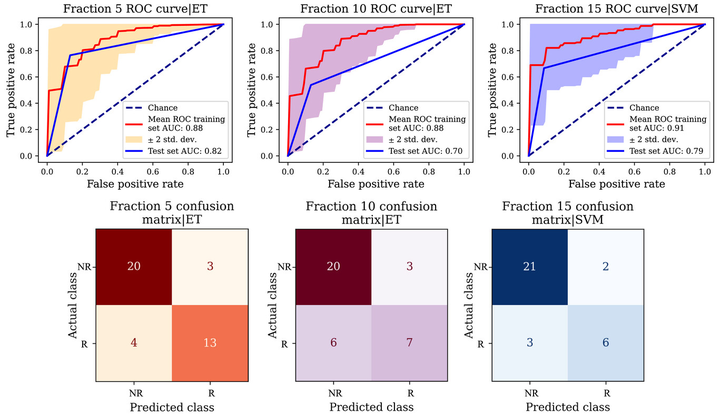 Image credit: John Kildea
Image credit: John KildeaAbstract
Background: Head and neck cancer (HNC) patients undergoing radiotherapy (RT) may experience anatomical changes during treatment, which can compromise the validity of the initial treatment plan, necessitating replanning. However, ad hoc replanning disrupts clinical workflows and increases workload.Currently, no standardized method exists to quantify anatomical variation that necessitates replanning..
Purpose: This project aimed to create geometrical metrics to describe anatomical changes in HNC patients during RT. The usefulness of these metrics was evaluated by a univariate analysis and through machine learning (ML) models to predict the need for replanning.
Methods: A cohort of 150 HNC patients treated at McGill University Health Centre was analyzed. Based on the shapes of the RT structures (body, PTV, mandible, neck, and submandibular contours), we developed 43 metrics and automatically calculated them through a Python pipeline that we called HNGeoNatomyX. Univariate analysis using linear regression was conducted to obtain the rate of change of each metric. We also obtained the relative variation of each metric between the pre-treatment and replanning-requested scans. Fraction-specific ML models (incorporating information available up to and including the specific fraction) for fractions 5, 10, and 15 were built using metrics, clinical data, and feature selection techniques. Model performance was estimated with repeated stratified 5-fold cross-validation resampling technique and the area under the curve (AUC) of the receiver operating characteristic (ROC) curve.
Results: Univariate analysis showed that body- and neck-related metrics were most predictive of replanning need. Our best specific multivariate models for fractions 5, 10, and 15 yielded testing scores of 0.82, 0.70, and 0.79, respectively. Our models early predicted replanning for 76% of the true positives
Conclusions: The created metrics have the potential to characterize and distinguish which patients will necessitate RT replanning. They show promise in guiding clinicians to evaluate RT replanning for HNC patients and streamline workflows.